Lung Transplant Program
Lung Cancer Rapid Assessment & Management Program (LungRAMP)
Benign Esophageal Disease (reflux, motility disorders)
Interventional Thoracic Surgical Suite
Surgery for Emphysema Program
Malignant Mesothelioma
Chronic Thromboembolic Pulmonary Hypertension (CTEPH)
Lung Metastases Program
Lung Transplant Program
“On behalf of my family, I would like to thank all the staff of the lung transplant program for their hard work, commitment and dedication to the well-being of their patients. I would say this is the Best Hospital in the World!” – UHN Patient
Our lung transplant program is the largest in Canada and we transplant patients with a variety of lung diseases including: pulmonary fibrosis, emphysema, cystic
Beginning with the world’s first successful lung transplant in 1983 and continuing with the first successful double-lung transplant in 1986, the program now performs between 80-100 lung transplants each year. In 2007 the program performed a landmark 100 transplants in that year. Recently the program completed the 1000th lung transplant since the inception of the program.
Many of our patients come from different parts of Ontario and other provinces. Our respirologists use a system called Telehealth (internet video conferencing) to assess and discuss transplantation with these patients, their support persons and their local health care professionals.
The lung transplantation process involves a multidisciplinary team. From consultation to transplant and follow-up, patients interact with a team that includes respirologists, thoracic surgeons, anaesthetists, advanced practice nurses (APN), transplant coordinators (who are also registered nurses), social workers, psychiatrists and psychiatric nurses, physiotherapists, nutritionists, and other specialists when necessary. Throughout the assessment process, transplant candidates and their family members are provided with information, so they can make an informed decision about whether transplant surgery is the right option for them.
If a physician would like to refer a patient to the lung transplant program, you may download the referral form and fax the information to the lung transplant assessment office. The patient should be at least 3 consecutive months smoke free, and if greater than age 70 have an accompanying recent echocardiogram and nuclear cardiac drug stress test. The referral package should also include relevant and recent clinic notes, PFT’s, and any recent imaging like a CT scan.
For more information and to download the referral form, please go to: http://www.uhn.ca/Focus_of_Care/MOT/Lung/index.asp
Referrals may be directed to:
Pre-Transplant office
Phone: (416) 340-4800 ext. 6834
Fax: (416) 340-3097
Lung Cancer Rapid Assessment & Management Program (LungRAMP)
The Lung Cancer Rapid Assessment & Management Program (LungRAMP) Funded by Cancer Care Ontario, the Lung Cancer Rapid Assessment & Management Program (LungRAMP) enables patients who are suspected of having lung cancer to obtain consultation and state-of-the-art diagnostic investigations through a streamlined process. The goal is to reduce wait times for appointments and diagnostic testing and decrease the number of clinic visits, shortening the time period to diagnosis. For example, in the first six months of 2014, over 400 patients reached a definitive diagnosis with an average wait time between referral and diagnosis of 28 days. Almost all patients are contacted within 24 hours and our Nurse Navigator reaches out within 48 hours.
Referrals from any community physician that presents with a suspicious Chest X-ray, CT-chest or positive pathology with or without clinical history such as hemoptysis, prolonged cough or recurrent pulmonary infections are received at a dedicated fax number 416-340-3353 where it is triaged and assigned to the specified thoracic surgeon or the surgeon with the earliest available OR time slot according to case urgency and complexity.
Within 24 hours, our administrative assistants will contact you. Our Nurse Navigator will contact you to take a clinical history and ensure that everything is being done to expedite your case and make your assessment and management process as smooth and supportive as possible.
Patient-centred care is our number-one priority. Our goal is to maintain and improve your quality of care by making the process of diagnosis and treatment more efficient and supportive, by reducing multiple visits, by clarifying each step of the your care experience, by providing information on demand and by reducing your anxiety. We regularly seek patients’ views on their experience at the clinic to help us continue to enhance our service.
The patient experience when lung cancer is suspected can be very confusing and frightening. We will do our best to help make this process as transparent as possible and support patients and their families through this difficult time.
Click here for helpful information explaining the lung cancer diagnosis pathway
Physicians and patients are welcome to contact our nurse patient navigator.
Click here for the referral form
Phone: 1-877-LUNG911 (586-4911) or (416) 340-5138
Fax a referral: (416) 340-3353
Your Patient Nurse Navigator
A cancer diagnosis has the power to produce a myriad of overwhelming emotional responses, including shock, denial, anxiety, fear, grief, and depression. A cancer patient’s footpath through the health care system involves dealing with this host of feelings while juggling a multitude of medical tests and consultations to determine a definitive diagnosis and course of treatment. Your Nurse navigator is here to make that journey easier.
The Patient navigator is an important bridge between the doctor, adjunct services, and the patient. He/she’s responsibilities include providing patient education, removing barriers to care, and ensuring tests and appointments are completed in a timely manner. The patient navigator offers psychological support and orient patients to other services that may help them cope. Your patient navigator is an important link between you and your medical team.
Patient Experience Survey
We are very interested in knowing what you think about your diagnostic journey with us.
Your diagnostic testing was done by a team of doctors and nurses who are here to give you the best care possible. Specifically, our patient navigator will have contacted you initially, and then most of the coordination will have been done by your surgeon’s administrative assistant.
We want to know what you think about the care you had from this team so that we can improve your care. This survey will help us understand the quality of care and make suggestions for improvements.
Your answers are meant to be anonymous and confidential. Your name is not required and hospital staff will not see your specific answers. The comments will only be seen in summary form. The survey will take about 5 minutes to complete.
You can skip any question that you do not want to answer. If you do not want to fill out the survey, your care will not be affected. By clicking here, you can complete the online survey.
Information on Tests & Preparation
Lung Cancer Diagnosis Patient Pathway
What You Need to Know About Biopsy
What to Expect When Having a Bronchoscopy
MRI Instructions for LungRamp Patients
Myocardial Perfusion Scan Persantine Thallium
Helpful Links
Click here for what you should know about Lung cancer
Click here for Smoker’s HELP LINE – Thinking of quitting?
Benign Esophageal Disease (reflux, motility disorders)
Benign esophageal diseases include hiatus hernia, gastroesophageal reflux, esophageal motility disorders, achalasia and non-malignant tumours of the esophagus. Many of these conditions can be treated with minimally invasive surgery or endoscopic therapies. Available endoscopic therapies include esophageal dilation, endomucosal resection and radiofrequency ablation.
Our benign esophageal disease clinic is held on Tuesdays at Toronto General Hospital. Once per month we have a multidisciplinary clinic with gastroenterology and general surgery for patients with complex esophageal problems including atypical symptoms, complex motility disorders, recurrent symptoms after surgery and persistent symptoms despite appropriate therapy. This clinic is followed by a multidisciplinary education round.
Through our program, you will receive care from surgeons and physicians specializing in these conditions.
Referrals may be directed to:
Dr. Andrew Pierre
Phone: (416) 340-5354
Fax: (416) 340-4556 or (416) 340-3353 Or
Dr. Gail Darling
Phone: (416) 340-3121
Fax: (416) 340-3660
Interventional Thoracic Surgical Suite
A new Interventional Thoracic Surgery Program was established within the Division of Thoracic Surgery under the direction of Dr. Kazuhiro Yasufuku, highlighted by the opening of a state-of the-art Interventional Thoracic Surgery Suite (ITSS) at the Toronto General Hospital in July 2010. The ITSS, first of its kind in Canada, is a hybrid endoscopy/surgical suite capable of general anesthetic equipped with state of the art endoscopy technology. The ITSS provides leading-edge thoracic interventional procedures such as diagnostic bronchoscopy (white light bronchoscopy, autofluorescence bronchoscopy, narrow band imaging, endobronchial ultrasound, transbronchial biopsy, navigational bronchoscopy, in-vivo endocytoscopy), airway stenting, photodynamic therapy, VATS pleuroscopy, management of pleural effusion and similar technology for esophageal diseases. ITSS will be integrated with our existing intervention programs in the Division of Thoracic Surgery: minimally invasive and ultra-minimally invasive surgery, image guided therapy, and basic research.
Referrals may be directed to:
LungRAMP (Lung Cancer Rapid Assessment and Management Program)
Phone: (416) 340-5138
Fax: (416) 340-3353
or
Kazuhiro Yasufuku MD, PhD
Director, Interventional Thoracic Surgery Program
Toronto General Hospital, University Health Network
200 Elizabeth St, 9N-957
Toronto, ON M5G 2C4 Canada
416-340-4290 (P)
416-340-3660 (F)
kazuhiro.yasufuku@uhn.ca
Surgery for Emphysema Program
Led by Dr. Thomas Waddell, and in partnership with the Pulmonary Rehabilitation Program at West Park Hospital, this program offers a comprehensive assessment program based on CT and other scans to identify those patients with severe emphysema that might benefit for surgery.
Emphysema is a chronic lung disease where patients develop shortness of breath, wheeziness and difficulty to exercise. For the most part, the treatment is medical, that is puffer medication and occasionally pills or supplemental oxygen.
Referrals should come from pulmonary medicine specialists to ensure all other medical treatments have been optimized.
Referrals may be sent to:
Dr. Thomas Waddell
Phone: (416) 340-3432
Fax: (416) 340-4556
Malignant Mesothelioma
Here at the Division of Thoracic Surgery, we have created a special program for patients with known or suspected mesothelioma, which is led by Dr. Marc de Perrot.
Malignant mesothelioma is a rare cancer which has been linked to asbestos exposure. This disease can occur in the pleura, which is the outer lining of the lungs and the internal chest wall or in the peritoneum, which is the lining of the abdominal cavity. Patients may develop shortness of breath, cough or chest pain. Some patients have no symptoms. Build up of fluid around the lungs is also common.
There are various treatment options for this disease, depending on the extent of disease and may include chemotherapy or radiation therapy possibly then followed by surgery.
Referrals may be directed to:
Dr. Marc de Perrot
Phone: (416) 340-5549
Fax: (416) 340-3478
Chronic Thromboembolic Pulmonary Hypertension (CTEPH)
Toronto CTEPH Program
The Toronto CTEPH Program receives referrals from physicians for patients who have suspected diagnosis of CTEPH. Led by Dr. de Perrot, the program offers multidisciplinary assessment by the surgeons and respirologists who have expertise in the field of pulmonary hypertension. Being the largest Canadian center for the pulmonary thromboendarterectomy (PEA) surgery, the program receives referrals from across the country.
Our Goals
• Evaluation of acute and chronic thromboembolic disease
• Education of patients and families about chronic thromboembolic pulmonary hypertension (CTEPH) and pulmonary thromboendarterectomy (PEA)
• Surgical management of CTEPH through PEA
• Increasing public and medical community awareness about CTEPH diagnosis and curative surgical treatment
• Clinical research
Our Team
• Dr. Marc de Perrot, Thoracic Surgeon
• Dr. John Granton, Respirologist
• Dr. John Thenganatt, Respirologist
• Dr. Jakov Moric, Respirologist
• Anastasia Bykova, Nurse Practitioner
• Susan Beaudoin, Clinical Coordinator
About CTEPH
CTEPH is a type of pulmonary hypertension that is caused by the unresolved or recurrent pulmonary emboli leading to chronic pulmonary vascular obstruction by an organized clot. The disease progresses despite adequate anticoagulation as a result of secondary arteriopathy eventually leading to the right heart failure and death. Recognition of CTEPH in patients with history of pulmonary emboli is important to achieve timely diagnosis and appropriate follow up/referral.
Patients with CTEPH can present with acute pulmonary emboli. CTEPH should be suspected in the presence of:
• Idiopathic and/or recurrent pulmonary emboli
• Longer time between symptom onset and diagnosis
• Right ventricular systolic pressure > 50 mmHg on echocardiogram
• Large perfusion defects, mosaic parenchymal changes, and/or arterial webs or bands on CT Pulmonary Angiogram
Who should be referred to the CTEPH center?
All patients with the history of pulmonary emboli who remain symptomatic with dyspnea despite 3 months of therapeutic anticoagulation should undergo a ventilation-perfusion scan (V/Q scan). If the ventilation-perfusion scan shows mismatched perfusion defects, patients should be referred to our center for definitive evaluation and treatment.
Considering that a proportion of patients with CTEPH do not have a history of pulmonary emboli, the presence of dyspnea with mismatch perfusion defects on V/Q scan should also warrant referral to our center for evaluate the possibility of CTEPH.
How to make a referral to the Toronto CTEPH Program?
When making a referral, please include:
• A letter of referral
• Clinical notes
• Reports of investigations (V/Q scan, CT thorax, echocardiogram, etc.)
Please fax referrals to 416-340-3853
Treatment for CTEPH
Pulmonary thromboendarterectomy is the treatment of choice for CTEPH. The PEA surgery leads to major clinical improvements due to improved hemodynamic parameters and oxygenation, and reduction in dead space ventilation. The surgery can be also curative in the large number of patients with resolution of the pulmonary hypertension. Majority of the patients experience significant functional recovery and are able to return to their baseline physical activity level without supplemental oxygen use.
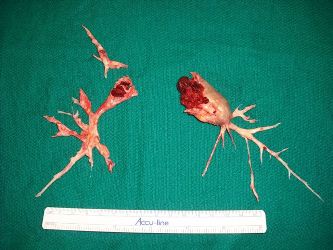
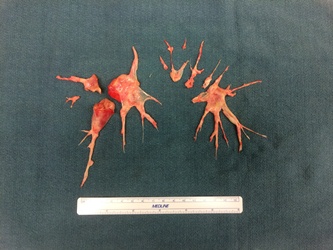
Article on “When to Refer a Patient With Chronic Thromboembolic Pulmonary Hypertension for Pulmonary Endarterectomy”
Article on “Pulmonary endarterectomy in severe chronic thromboembolic pulmonary hypertension”
Article on “Chronic Thromboembolic Pulmonary Hypertension: Curable Type of Pulmonary Hypertension” English Version
Article on “Chronic Thromboembolic Pulmonary Hypertension: Curable Type of Pulmonary Hypertension” French Version
Booklet for health professionals about CTEPH diagnosis and management
Click here for PHA Canada Website
Contact Information
Toronto CTEPH Program
Division of Thoracic Surgery – 9N927
Toronto General Hospital
200 Elizabeth Street
Toronto, ON M5G 2C4
Phone: 416-340-4800 ext 5274
Fax: 416-340-3853 (for referrals)
Pager: 416-714-0840
Click here for more patient information
Lung Metastases Program
Many patients with cancer develop secondary tumours in the lungs or other organs (metastasis). When these occur in the lungs and only in the lungs, there may be a possibility to remove or destroy them.
The Division of Thoracic Surgery in collaboration with the Radiation Medicine Program has developed The Lung Metastectomy Program.
Our highly specialized diagnostic and management service enables patients with cancer of any primary site other than the lungs and that has spread to the lungs (lung metastasis) to obtain consultation and diagnostic investigations to assess surgery or radiotherapy as treatments for lung metastasis. Our goal is to prolong life and improve quality of life by offering a multidisciplinary assessment and cutting-edge surgical or radiation therapy treatment in the most efficient and supportive way. This highly specialized diagnostic and management service assesses patients with cancer of any primary site other than the lungs where the cancer has spread to the lungs (lung metastasis) to assess surgery or radiotherapy as treatments for lung metastasis.
Referrals from oncological and surgical specialists with patients that have a primary cancer in any site other than lung and present with lung metastasis are triaged and scheduled to the earliest available clinic appointment according to case urgency and complexity. The Referring Physician and primary oncology nurse who have followed the patient during their initial treatment will be contacted by our staff to gather a detailed clinical history and imaging. All cases will be reviewed by a multidisciplinary group on the day of consult to assess each case and plan management & treatment. The referring physician and primary oncology nurse are invited to participate in this review.
The Clinic is held at Princess Margaret Hospital (2nd floor – Lung Clinic)
For consideration at this clinic, referring oncologists should contact the coordinator.
Contact Information:
Marlene Dador
Phone: (416) 340-4800 ext. 6324 or (416) 340-4800 ext. 6992
Fax: (416) 340-3353
